Every day, 120 Americans commit suicide; 20 of them are war veterans.1 2 “I know without a doubt: MDMA saved my life.” said one war veteran who was suffering from post-traumatic stress disorder (PTSD), a mental condition which is hard to cure and may lead to further disorders such as anxiety, depression and addiction.

More than 868,000 US war veterans suffer from PTSD and their families suffer with them.3 Living with a partner or parent with PTSD means living with their elevated levels of anger or irritability which are often paired with feelings of hopelessness, guilt or depression and all too frequently accompanied with substance abuse. At best, this poses a challenging family life, at worst it can lead to suicide. As dark as this situation may be, a new ray of hope is emerging from—of all things—MDMA: a substance currently deemed an illegal party drug. MDMA-assisted therapy has proven to be far more effective than any other PTSD treatment available today. The Food and Drug Administration (FDA) has approved a roadmap to legalize the substance for medical use by 2021.
MDMA is currently being researched for its efficacy in social anxiety, end-of-life distress, couples therapy and most pressingly: PTSD. Consider that more US troops die from suicide than in combat. Besides the emotional costs of such a condition, an estimated $17 billion are spent on disability compensation for veterans suffering from PTSD each year.3
Unlike common psychiatric medicine, that has to be taken on a daily basis and potentially for the rest of one’s life, MDMA is only administered a few times. According to the latest study by MAPS, after only three sessions of MDMA-assisted therapy, 61% of patients no longer suffered from PTSD.4 The effects are immediate and long-lasting; an earlier study showed that even after four years later the patients did not tend to relapse.5
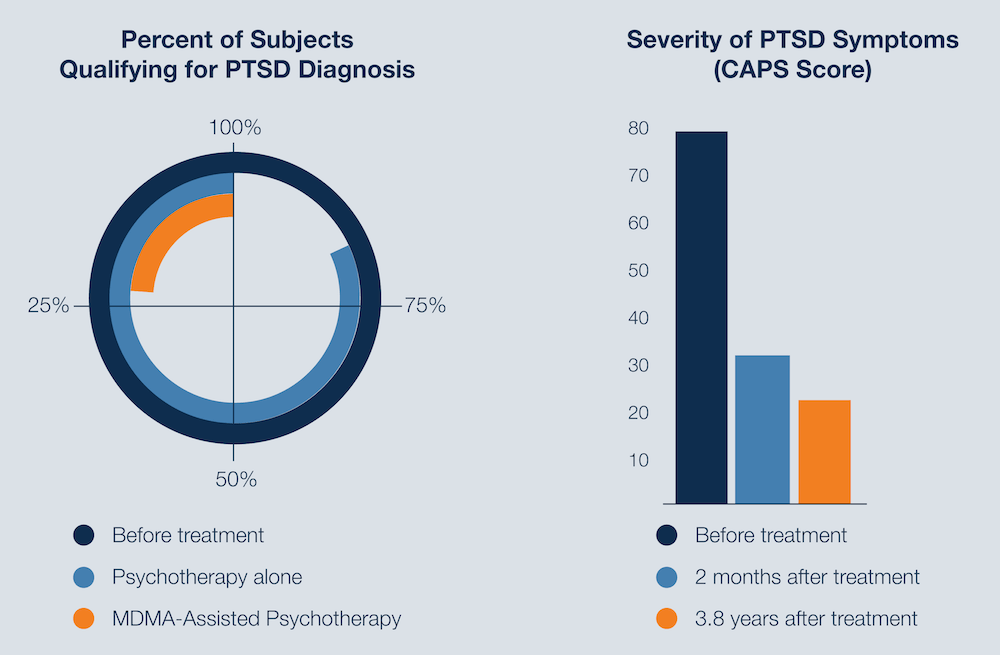 MAPS study results. Snippet from MAPS infographic on PTSD
MAPS study results. Snippet from MAPS infographic on PTSD
What these numbers don’t reflect are the dramatic stories of the war veterans, rape survivors and victims of childhood abuse behind these statistics. For years, they had lived with chronic anxiety, depression and panic attacks until they finally underwent MDMA-assisted therapy. Scott, who served in Afghanistan and Iraq and had seen three of his comrades commit suicide, said “I know without a doubt: MDMA saved my life.” Watch some of the study participants tell their story in their own words. You might want to keep a tissue handy.
What is trauma?
“Trauma is not a divorce, your mother’s depression, your father’s alcoholism or physical abuse.” explains Dr. Gabor Maté, psychiatrist and expert in trauma, addiction and ADD. While such experiences may be traumatic, they’re not the trauma itself. He emphasizes that “Trauma is not what happens to you, trauma is what happens inside you.”6 And what may happen inside of you as a result of a traumatic event is that you get disconnected from your emotions and your body. This in turn makes it increasingly difficult for you to be present in the moment. You develop a negative view of the world, of yourself and you develop a defensive attitude towards other people. 6
“Trauma isn’t what happens to you, it’s what happens inside you.”
And indeed, people suffering from PTSD often find it difficult to regulate their emotions and navigate relationships. The typical clinical symptoms of PTSD are insomnia, anxiety, nightmares, emotional distress or panic attacks. 7
Post-traumatic stress disorder in the brain
How does PTSD manifest in the brain? People who suffer from PTSD show a decreased activity in the hippocampus and the prefrontal cortex—areas associated with learning, rational thinking and decision making. At the same time, a brain area called the amygdala—responsible for emotions, fear conditioning and fight-or-flight responses— shows increased activity levels. The amygdala is the commander-in-chief of your survival instincts. When she speaks, everybody listens.
 Snippet from MAPS infographic on PTSD
Snippet from MAPS infographic on PTSD
Now, when a PTSD patient is reminded of a traumatic experience—through subtle cues like sounds, smells or fabrics—their amygdala takes over and shuts down the higher order functions of their brain, like the prefrontal cortex. The individual is left with a seemingly irrational fear response that can manifest as stress, panic or aggression. People who suffer from PTSD have the hardest time processing their trauma rationally, because whenever they’re confronted with their traumatic experience, the rational areas of their brains are simply not accessible.
MDMA helps navigating trauma
MDMA can help patients with PTSD to revisit their traumatic experiences without being overwhelmed by negative emotions. MDMA decreases activity in the amygdala8 and leaves the prefrontal cortex online, enabling patients to analyze and reflect on their experiences, which in turn gives them the chance to integrate these experiences into their lives.
A rape survivor described it as “It was like I got to do brain surgery on myself. I could go into my mind and see the thought patterns and the belief systems that had calcified in there and rewire them.”9
The right dose of MDMA puts patients in a so-called optimal arousal zone. That’s a state in which the patient is positive and calm while at the same time being motivated to engage in a therapeutic process and open to connect. Usually, patients suffering from PTSD struggle to be any of the above. They tend instead to be hypervigilant, closed up and reluctant to talk about their experience. For all these reasons, MDMA-assisted therapy is beginning to look like a fast lane to healing trauma.
Integration, integration, integration
MDMA alone doesn’t cure patients of their PTSD, it’s the combination of the substance and psychotherapy. The leading research organization in this field, MAPS (Multidisciplinary Association for Psychedelic Studies), uses a 12-week treatment protocol that distinguishes between three kinds of sessions: (1) preparation sessions, (2) dosing sessions and (3) integrative psychotherapy sessions.
 Treatment rooms have a cosy, living-room style atmosphere
Treatment rooms have a cosy, living-room style atmosphere
It’s of the utmost importance that patients feel safe and at home with their therapist. Not having a trusted ‘sitter’ was found to be one of the strongest predictors of a so-called bad trip.10 During preparation sessions, patient and therapist get to know one another and get comfortable with the setting. The dosing sessions usually include two therapists: ideally one male and one female. The star therapist-team in the MAPS studies were psychiatrist Michael Mithoefer and psychiatric nurse Ann Mithoefer, who is Michael’s wife. They are professionals with years of experience and training in special techniques such as Holotropic Breathwork, which Stanislav Grof developed based on decades of learnings from LSD-assisted therapy.
 Michael and Annie Mithoefer, therapists at MAPS
Michael and Annie Mithoefer, therapists at MAPS
During an MDMA dosing session, people are capable of accessing subconscious content that would usually be filtered or blocked out by their normal waking state of consciousness. When this door opens, patients can go through intense outbursts of emotions like sadness, desire or fear and often have meaningful insights. After the acute effects of the substance have tapered off, the therapist helps the patient to integrate their experience. This means helping the patient to acknowledge and allow their feelings, and as a next step, reflect on them in a self-compassionate way. If, as Dr. Gabor Maté proposes, trauma is the disconnection from one’s body and emotions, then integration is one’s re-connection to them.
Integration is one’s re-connection with their body and emotions.
Can MDMA fix your relationship?
Relationships are hard. The daily grind of bills, chores and raising children takes a toll on most every couple. Over time, misunderstandings and communication pitfalls turn into negative behavior patterns and—fast forward ten or twenty years—what used to be love may have turned into mere (dys)functional co-habitation.

For many couples this ends in either a loveless marriage or divorce. Preliminary studies have shown that MDMA-assisted therapy can help couples quickly get to the bottom of their problems and work through them. This is what we know so far:
MDMA helps the couple remember their initial feelings of love and deep connection to one another and thereby creates a safe space in which “you can say anything” as one study participant described.11 In an environment where one can be vulnerable, couples begin to talk openly about their sexual fantasies, their insecurities, their needs and desires. One woman even confessed that she had cheated on her husband. In their exceptionally open and accepting state, the couple managed to deal with her affair in a compassionate way which eventually resulted in strengthening their bond.11
With fear, defensiveness and resentment out of the way, couples are afforded a “nice clean slate” from which they can tackle their problems.11
To be clear, the idea is not to use MDMA regularly to be in a better mood with your partner. But a few strategically placed sessions can create enough momentum to permanently change relationship dynamics. A couple from another study stated that their MDMA sessions have torn down the barriers between them so they can talk more freely when sober.12 MDMA doesn’t fix your relationship. “It’s not a magic bullet. It’s how you integrate what you learn into your life.” explained a male participant from the same study. When he and his wife get into a conflict nowadays, rather than mindlessly arguing they ask “What is this really about?”.12
I’ve personally interviewed a number of couples who have used MDMA to work through tough phases in their relationships. What I’ve heard over and over again was “I don’t know if we’d still be together if it weren’t for MDMA”.
MDMA-assisted couples therapy
When couples seek out professional help they’re usually on a hair-trigger with one another, quite possibly already considering divorce. The clock is ticking, and what they need is immediate relief.
A few intentionally placed MDMA-assisted therapy sessions can be exactly the kind of drastic intervention that’s necessary. Several couples have told me “if done well, such a session can be like years of counseling”.
Currently, the focus of MDMA-assisted research lies in the treatment of trauma. The use of MDMA for couples therapy is an under-researched field and to my knowledge is practiced only in the underground or on a couple’s own accord, without the supervision of a therapist. While the lack of a therapist is certainly not ideal, the much bigger problem is the health risk associated with the use of an unregulated substance. Whereas a correctly measured dose of pure MDMA is relatively safe and has a lower toxicity profile that legal drugs like alcohol or cigarettes13—acquired from the black market, the user has no gauge of purity, correct dosage or possible contamination with harmful additives. The danger comes not with the use, but with the criminalization of MDMA.
Currently, our society is operating on a double standard. Have you ever been to a Christmas party without a bar? We allow alcohol as a means to bond with our co-workers. But we forbid MDMA as a means to mend our personal relationships.
The medical case for MDMA is strong and over the coming years, we will see country after country legalize the substance for therapeutic use. I can see a future in which therapists might add MDMA-assisted marriage counseling or MDMA-assisted family reconciliation to their portfolio. Personally, I’d certainly take advantage of such an offering.
This is the final article in my 7-part series on psychedelic drugs.
Medical Benefits of Psychedelic Drugs
Psychedelic Drugs and the Serotonergic System
The Psychedelic Experience
Your Brain on Psychedelic Drugs
Psychedelics and Mental Health
Microdosing LSD: Smart Drug or Placebo?
MDMA-assisted Therapy
Final Thoughts
The research I’ve done while writing this series has convinced me that psychedelic substances will fundamentally transform our approach to mental health. Some of the most reputable universities in the world—Imperial College London, Johns Hopkins, NYU—are leading modern research in psychedelics. They have produced staggering results which have encouraged yet further institutions to engage in this re-emerging field of research. For the first time, we see more publications on psychedelics today than we saw in the 1960s.
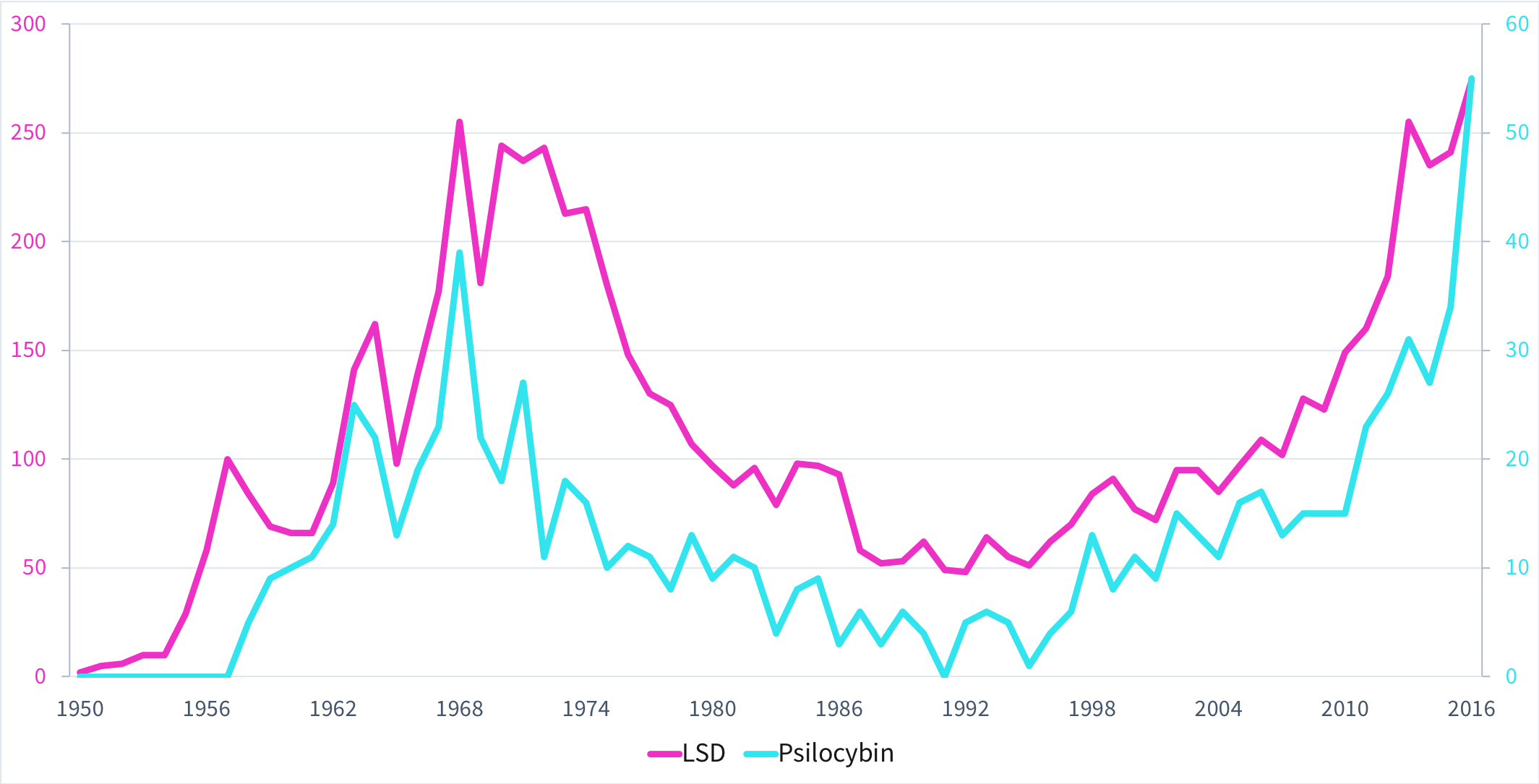 Number of scientific articles on PubMed. Medline trend ©Alexandru Dan Corlan
Number of scientific articles on PubMed. Medline trend ©Alexandru Dan Corlan
But it’s more than data and science. I’ve now met many of the people behind this so-called psychedelic renaissance and I’ve found them to be incredibly smart, caring and passionate. Indeed, their work has inspired me to make my own contribution. In May 2017, I founded the Psychedelic Society Vienna to start an evidence-based conversation about the true risks and benefits of psychedelic substances. We run events, workshops and integration circles and work towards bringing psychedelic research to Austria. Our community is growing rapidly and has brought many wonderful people and meaningful friendships into my life. Thank you all!
References
-
United States: Suicide Injury Deaths and Rates per 100,000. (All Races, Both Sexes, All Ages). 2016. CDC. Retrieved on 2018-03-03 via WISQARS Fatal Injury Reports. ↩
-
National Suicide Data Report. 2016. U.S. Department of Veteran Affairs. ↩
-
Rick Doblin. Opening Plenary: Psychedelic Science 2017. 2017. Youtube. ↩ ↩2
-
A Phase 3 Program of MDMA-Assisted Psychotherapy for the Treatment of Severe Posttraumatic Stress Disorder (PTSD). MAPS. Retrieved 2018-03-01. ↩
-
Infographic MDMA-assisted therapy for PTSD. MAPS. Retrieved 2018-03-01. ↩
-
Dr. Gabor Maté — New Paradigms, Ayahuasca and Redefining Action. The Tim Ferriss Show. 2018. ↩ ↩2
-
Psychological trauma. Wikipedia. Retrieved 2017-10-19 ↩
-
Carhart-Harris RL, Murphy K, Leech R. The Effects of Acutely Administered 3,4-Methylenedioxymethamphetamine on Spontaneous Brain Function in Healthy Volunteers Measured with Arterial Spin Labeling and Blood Oxygen Level-Dependent Resting State Functional Connectivity. Biol Psychiatry. 2015 Oct 15;78(8):554-62. PubMed PMID: 24495461. PMCID: PMC4578244. ↩
-
MDMA – The Movie 2015. Youtube. ↩
-
Carbonaro TM, Bradstreet MP, Barrett FS et al. Survey study of challenging experiences after ingesting psilocybin mushrooms: Acute and enduring positive and negative consequences. J Psychopharmacol. 2016 Dec;30(12):1268-1278. Epub 2016 Aug 30. PubMed PMID: 27578767. ↩
-
Katie Anderson. MDMA’s impact on romantic relationships. 2016. Youtube. Retrieved 2018-02-28 ↩ ↩2 ↩3
-
Cat McShane. Refinery29: The Couples That Take MDMA To Stay Together. 2017. MAPS. ↩ ↩2
-
Nutt DJ, King LA, Phillips LD; Independent Scientific Committee on Drugs. Drug harms in the UK: a multicriteria decision analysis. Lancet. 2010 Nov 6;376(9752):1558-65. doi: 10.1016/S0140-6736(10)61462-6. Epub 2010 Oct 29. PubMed PMID: 21036393. ↩